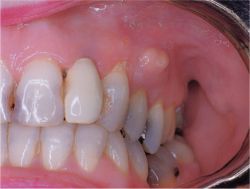
Children periodontitis
The structure of dental caries disease complications account for about 35-50% of all cases of requests for dental care. The number of caries complications, including periodontitis, is constantly high, even among the urban population of Russia. And worse than organized sanitation, the more frequently diagnosed with inflammatory periodontal disease.

Periodontium is located in the space bounded on one side of the cortical plate wells, on the other - the root of the cement. Feature of periodontal unformed tooth is that, extending from the neck of the tooth to form part of the root and merging with the growth zone, it is in contact with the pulp canal. As formation of the root zone of the size of the sprout and the apical foramen contact with the pulp are reduced, and periodontal ligament length increases. After the end of the root apex as far back as the year continues to develop periodontal. As the root resorption of temporary teeth periodontal ligament length decreases and the contact with the pulp and periodontal cancellous bone increases again.
During the period of temporary tooth root resorption at the site of its adjacency to the rudiment of constant cancellous and cortical plate, bounding the gap, and periodontal root cement, dissolve, which leads to the disappearance of periodontal at this site.
The absence of a stable structure and the thickness of the periodontium in the apical part is the anatomical and physiological features during the development and formation of the roots of temporary and permanent teeth.
Periodontium in the child presented a rather loose connective tissue and contains a large number of cellular elements and blood vessels, which accounts for its reactivity when exposed to adverse factors.
The primary cause of periodontal disease in children is when micro-organisms, their toxins, biogenic amines, coming from the inflamed necrotic pulp are distributed in the periodontium.
Second place goes to the tooth trauma: injury, dislocation, fracture of the root at some level. In this case we are talking mainly about the front teeth. Young children, toddlers, fall face down, resulting in different types of partial dislocations, including vkolochennyh, often accompanied by rupture of a neurovascular bundle. At school age, are often permanent injury immature anterior teeth. If children do not seek help, the pulp gradually, without marked clinical manifestations, dies, and develop chronic periodontitis. A role in periodontal disease may play a mechanical trauma during root canal treatment sharps, needles, or drilborami during injection of filling material over the top.
A role in the development of periodontitis in children are strong chemical and medicinal substances that penetrate into the periodontium in the treatment of pulpitis. Often there are cases of periodontitis, especially in the frontal teeth of the upper jaw, because of the reluctance to use insulating pads when working with evikrolom.
Reducing the time of treatment of patients with pulpitis by reducing length of stay of mummified in the oral cavity leads to the further progression of the disease process, the transition of a single nosologic entity to another. Was also found that 20% of the occurrence of periodontal disease was caused by the prolonged treatment of teeth with pulpitis, especially in cases plohoprohodimyh channels. In this case violated the rules of endodontic treatment channels, but since the method allows replacement of mummified devitalization of the antibiotics, enzymes, etc. In 4% of patients with periodontitis was caused by errors or complications during treatment: perforation of the bottom cavity of the tooth or root canal in the presence of endodontic instrument fragment, excessive excretion of filling material in zaverhushechnuyu area and 6% - incomplete root canal fillings. In 2% of patients with periodontal disease occurrence was associated with prolonged use of arsenic prepaoatov.
Thus, in 41% of cases due to the emergence of periodontitis iatrogenic factors. In rare cases, periodontal inflammation may develop hematogenous route with acute infectious diseases of children. Possible way of spreading the infection to the periodontium per continuitatem from inflamed tissues, in the neighborhood.
Features of the appearance and character of the course of inflammatory processes in the periodontium, but the direct etiologic factors are largely determined by local and also the general level of resistance. Such co-acute and chronic diseases such as flu, sore throat, gastrointestinal tract, etc., reduce the protective capacity and immune reactivity of the organism, creating conditions for the occurrence of acute and chronic periodontitis.
Of periodontitis exhibit different associations of microorganisms. In the composition of the microflora is dominated by grampolo of positive-negative cocci (mainly staphylococci and streptococci) and yeasts, lactobacilli, actinomycetes, etc. Among the most frequently isolated microorganisms in the first place - aerobic and anaerobic species of streptococci, and then - staphylococci.
In the diagnosis of chronic periodontitis temporary teeth in children can not be limited only by clinical data. Understanding of the nature of the inflammatory process and the extent of its influence on the permanent tooth bud give X-ray data. It must be done not only in the event of various complications of the inflammatory process, but before any treatment of a tooth with chronic periodontitis, as even during quiet clinical course of inflammation can be detected radiographically severe complications, changing treatment policy.
Of particular value in addressing this issue in pediatric practice of utilizing well-proven method of panoramic radiography. In a short time and at low doses of radiation it gives much information about the state of the periapical tissues of teeth, can identify the correct remedial measures to avoid complications, etc.
Classification of periodontitis
On the basis of isolated etiological infectious, traumatic and drug periodontitis. By location - apical and marginal. Downstream of the pathological process are acute (serous and purulent), and chronic (fibrosis, granulating, granulomatous), and exacerbated chronic periodontitis. Periodontitis is marginal, marginal, or if the inflammation is primarily originated from the gingival margin. The cause of his injury is often the gingival papillae in pencil, food, sharp-walled cavity, the edges of the crown. Prolonged irritation of the gums promotes the progression of acute inflammation in chronic marginal.
Acute apical periodontitis
The clinical picture of acute and pathoanatomical periodontitis temporary teeth is basically the same as permanent. However, the anatomical features of the temporary teeth are responsible for some originality in the development of acute periodontitis: in connection with a wide opening in the apical periodontium during formation or resorption of the roots of pulp inflammation is readily converted to the periapical tissue. Sometimes periodontitis develops earlier than the inflammation encompasses the entire root pulp. More severe periodontal disease and tooth temporary transition of the inflammatory process in the surrounding soft tissue and bone is associated with reduced resistance to the child's body.
In acute apical periodontitis children complain of pain expressed by the ever-increasing, with pressure growing on the tooth. The child indicates exactly a bad tooth. The next important symptoms are swelling of the gums and surrounding soft tissue swelling and an increase in regional lymph nodes, sharply painful percussion of the tooth. In temporary teeth acute periodontitis develops very rapidly and, if not created by the outflow of fluid, infection is spreading rapidly across the jaw bone, causing the abscess. In young children, in response to inflammation of periodontal growing general signs of intoxication: increased temperature, increased sedimentation rate and leukocytosis.
Acute apical periodontitis in children is rare, it must be differentiated from exacerbation of chronic periodontitis. The clinical picture of both diseases may be identical, but in acute periodontitis in the radiograph is no deviation from the norm, and an exacerbation of chronic periodontitis radiographically well-defined characteristic changes.
Prevention of acute periodontitis is an early, timely and proper rehabilitation of the teeth with pulpitis. Acute apical periodontitis can result in recovery and transition to the chronic form, and in case of increase of the inflammatory process - the development of periostitis or osteomyelitis.
Chronic periodontitis
In children, the inflammatory processes in the pulp and periodontium are closely linked. More than 30% of chronic periodontitis occurs when the incorrect treatment of teeth with pulpitis, about 38% - with the development of caries without treatment and about 30% - due to injury. Children 6-8 years chronic granulating periodontitis develops as a result of permanent injury immature incisor teeth (usually the top jaw) and due to decompensated acute course of caries in first molars. Chronic periodontitis develops as a result of acute apical periodontitis or chronic primary process as a result of chronic pulpitis. Picture in pathology of chronic periodontitis is dominated by the phenomenon of exudation are not as acute process, and proliferation: growth of fibrous or granulation tissue.
Chronic periodontitis in temporary and permanent teeth often immature in the presence of a shallow cavity in the absence of communication with the cavity of the tooth. This is due to anatomical features of the structure of hard tissues of temporary and permanent teeth with incomplete root formation.
Chronic periodontitis fibrotic
Complication arises as a result of pulpitis, periodontitis, acute and chronic treatment after granulating and granulite lematoznogo periodontitis. Develops only in teeth with formed roots (both temporary and permanent teeth). During the formation of the tooth, in the absence of a stable structure in the apex of the root, and root resorption during the temporary teeth fibrous periodontitis is not observed. Clinically, fibrous periodontitis is not accompanied by any symptoms and are sometimes found incidentally during dental X-ray system. There are no complaints, percussion painless, gum normal color of the tooth mobility is not detected. Sometimes the color of the tooth crown, he becomes more dull with a grayish or bluish tint.
Diagnosis is based on X-ray: fibrous thickening of periodontitis is characterized by periodontal and seal, as evidenced by extensive periodontal crevice. The width of periodontal ligament varies in a limited area or, less frequently, throughout the periodontal space, which depends on the extent of the inflammatory process.
Chronic periodontitis fibrous differentiate from secondary caries, chronic gangrenous pulpitis, to a lesser extent - from deep caries. Similar to chronic periodontitis fibrous X-ray pattern is observed at a time when the formation of the root apex over and over, the periodontal gap is physiologically enhanced. Increased periodontal ligament noted also in some types of partial dislocation of the stylus in the direction of the adjacent tooth. In this case, the gap narrowed periodontal on the side where the tooth was displaced, and extended from the opposite side of the displacement.
Chronic granulomatous periodontitis
As chronic fibrotic, granulomatous periodontitis in temporary teeth is rare. Develops mainly in permanent teeth with roots formed, asymptomatic, rarely formed a fistula in the area of the damaged tooth. Typically, cavities are not in communication with the cavity of the tooth. On X-ray revealed granulomatous periodontitis in the form of focal destruction of bone tissue round or oval at apex with clear contours up to 5 mm (Fig. 4). Bone tissue around the granulomas are usually not changed, at least on its edges visible sclerosal compacted zone delimited bone of normal structure. The presence of multiple sclerosis indicates the reaction of the bones with prolonged duration of the inflammatory process. Periodontal gap bounded by the cortical plate, there is not throughout the root. The tip of the tooth root, which is located in the granuloma, often not resorbed.
Differentiate chronic granulomatous periodontitis should be of secondary caries, chronic gangrenous pulpitis, and other forms of periodontitis, kistogranulemy, cysts and partial dislocation of the tooth towards the occlusal plane. Radiological case of incomplete dislocation in the direction of the occlusal plane is visible deserted part of the alveoli, resembling a granuloma. Some natural openings (copperplate, mental) are projected on top of the root, mimicking granuloma. In permanent teeth immature granuloma should be differentiated from the emerging growth areas of the tooth. Sprout area bounded continuous cortical plate. At granulite lematoznom periodontitis periodontal gap is uneven width, in the apical part of the root extended. Cortical bone can be traced only to that portion of the root, from which to begin the expansion of periodontal ligament.
Chronic granulating periodontitis
The most common periodontal inflammation temporary teeth becomes chronic granulating periodontitis. Most often the disease is asymptomatic in a shallow cavity, and this causes difficulties in diagnosis because the clinical picture resembles the average caries. Sometimes patients may complain of pain during eating, bite sensitivity, discomfort or bloating in the patient's tooth. Necessary) to catch the child's response to some of the pain arising from the dissection of the cavity to aid in the diagnosis and differential diagnosis.
Granulating periodontitis form of temporary teeth is accompanied by the formation of a fistula with a detachable or the appearance of granulations protrudes on the gums, skin podnizhnechelyustnoy area, cheeks.
The appearance of the mouth of the fistulous on the face leads to the development of inflammation in his circle. The skin around the fistula hyperemia, eventually becomes bluish-cyanotic hue, macerate, thinner. From the mouth of the fistula can vybuhaet granulation. In the transition of the inflammatory process on the underlying fatty tissue there is an inflammatory infiltrate, usually 1-2 cm in diameter.
Fistula can be closed temporarily in initiating the outflow through the ruined ekssuddata crown and reappear, sometimes in a new location on the skin. Sometimes a well-defined palpates cord coming from the mouth of the fistula to the broken tooth. This strand is Svishchev course, around which gradually developed a large amount of connective tissue.
This picture served as the basis for the designation of the process as "migrating granuloma." This definition is sometimes found in the literature, and as an independent nosological form. In modern classifications of diseases, manuals and textbooks such nosologic entity does not exist, what is legitimate, since it is only a manifestation of periodontitis. Do not include the etiology and pathogenesis of this process - means to provide patient care inadequate. A similar pattern is observed on the face with dermal and subcutaneous forms of actinomycosis.
The predominance of granulation forms of periodontitis and recurrence of fistula associated with anatomical features of the structure of bone in childhood. If the fistula is not located in the projection of the root apex, and closer to the gingival margin, then it may be associated with a significant degree of dispersal or undeveloped roots. The same is observed in the localization of the inflammatory process at the bifurcation of the roots. Root resorption of temporary teeth can accelerate, slow down or stop. The rest of the apex of the tooth is often a temporary wall perforates the bone, thinning of the inflammatory process, and injures cheek or lip, which leads to the formation of ulcers dekubitalnoy. Such a temporary tooth to be removed.